Advancements in PAOO Techniques
In recent years, periodontally accelerated osteogenic orthodontics (PAOO) has seen remarkable technological advancements, leading to improved patient outcomes. This approach combines orthodontic techniques with minor surgical procedures to expedite tooth movement.
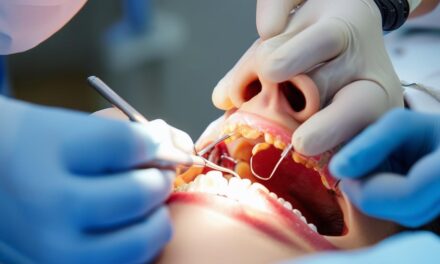
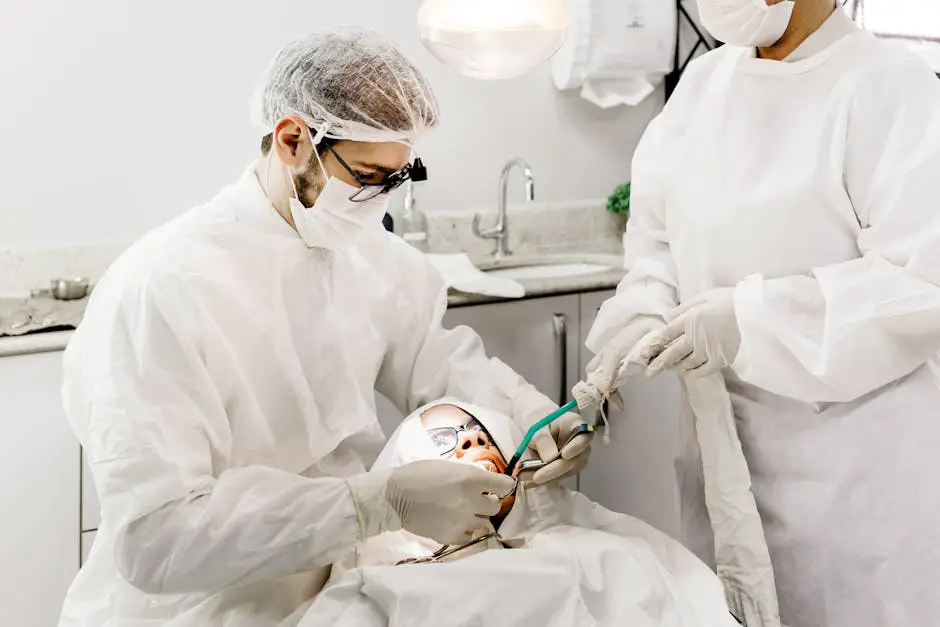
Surgical tools like piezoelectric devices create precise corticotomy cuts with minimal damage to surrounding tissues. These tools operate with ultrasonic frequency, targeting bone without harming soft tissues, ensuring quicker recovery times.
Innovative materials such as allograft bone grafts, like Maxxeus®, provide strong support while integrating seamlessly with the patient's bone. These materials, often combined with leucocyte-platelet-rich fibrin (L-PRF), enhance bone regeneration.1 Creating "Sticky Bone" using L-PRF stabilizes the graft and boosts healing, reducing the risk of complications.
Protocols now include comprehensive preoperative assessments with CBCT scans, enabling precise planning and customization of treatments. Detailed imaging helps orthodontists map out the exact movement required and the optimal points for corticotomy, ensuring targeted and effective interventions.
Timing is crucial in PAOO. Surgeons and orthodontists aim to initiate orthodontic force within a specific window—typically no later than two weeks after surgery. This timing leverages the regional acceleratory phenomenon (RAP) to maximize the speed of tooth movement.2 Quick adaptation to larger archwires post-surgery capitalizes on this brief period of heightened bone turnover.
Pain management protocols have been refined. Short-term steroid use and careful pain management post-surgery ensure patients experience minimal discomfort. While long-term use of nonsteroidal anti-inflammatory drugs is discouraged, immediate postoperative care focuses on patient comfort and reducing inflammation through ice packs and monitored medication.
Emerging research has showcased the benefits of combining PAOO with modern orthodontic appliances like Invisalign®. Using clear aligners post-surgery offers a discreet and comfortable method for directing tooth movement. This combination leverages PAOO's accelerated movement benefits while maintaining the aesthetic advantages of Invisalign®.
Incorporating comprehensive follow-up care minimizes relapse risks. Regular check-ups and maintenance sessions are crucial to monitor progress and maintain the alignment achieved through PAOO. Patients are educated on the importance of oral hygiene, given the increased pace and intensity of treatment.
The introduction of bioresorbable membranes in PAOO has been a game-changer. These membranes support the graft material during initial healing and gradually dissolve, eliminating the need for a second surgery to remove them. The use of materials like Pericardium® membranes supports bone regeneration while reducing patient discomfort and optimizing healing.
The ever-changing landscape of PAOO promises continued advancements, aiming to streamline procedures and further enhance patient outcomes.
Clinical Outcomes and Benefits
The clinical outcomes observed with the latest PAOO techniques have been transformative for patients seeking effective and efficient orthodontic solutions. One of the most significant benefits is the dramatic reduction in treatment times. With PAOO, treatment duration can be significantly shortened, sometimes by as much as two-thirds. This is particularly advantageous for adult patients who are keen to avoid the extended commitment typically required for orthodontic treatment.
The enhanced bone density achieved through PAOO is a game-changer. By utilizing innovative materials like Maxxeus® allograft bone grafts combined with L-PRF, the procedure supports accelerated tooth movement and fortifies the bone structure.3 Patients experience a strong and resilient periodontal framework, which is crucial for long-term dental health. This improvement in bone density also contributes to greater stability post-treatment, minimizing the risk of orthodontic relapse.
Enhanced periodontal health is another cornerstone of PAOO's success. The integration of bone grafting materials and advanced surgical techniques ensures that the periodontium remains strong and healthy. This is essential for preventing common orthodontic concerns such as bony defects and gingival recession.
One compelling case study involves a 23-year-old woman with a Class I malocclusion and severe crowding in her lower anteriors. Through PAOO, she achieved remarkable results within just over 7 months. The combined use of decortications and allograft bone grafting resolved her periodontal concerns and aligned her teeth efficiently.
Research supports the efficacy of PAOO. A meta-analysis published in Head & Face Medicine in 2024 demonstrated that PAOO significantly reduced total treatment duration and increased bone thickness compared to traditional orthodontic treatments.4 This evidence underscores the clinical effectiveness of PAOO, fostering greater acceptance of this method among practitioners and patients.
Follow-up care is integral to the success of PAOO. Patients are routinely scheduled for check-ups to monitor progress and ensure the stability of the orthodontic results. These appointments are essential for addressing any emerging issues promptly and maintaining the health of the periodontium. Educating patients on proper oral hygiene and the significance of regular dental cleanings further contributes to the long-term success of the treatment.
The advancements in PAOO reflect a harmonious blend of surgical precision and orthodontic expertise. This synergy optimizes clinical outcomes and enhances the patient's experience. The future of orthodontics is bright, with PAOO at the forefront, promising faster, safer, and more effective treatment options that prioritize patient comfort and long-term oral health.
Integration with Invisalign
Pairing periodontally accelerated osteogenic orthodontics (PAOO) with Invisalign represents a groundbreaking approach to modern orthodontic treatment. Patients benefit from the strengths of both techniques—the extensive potential for accelerated tooth movement of PAOO and the elegance and convenience of Invisalign's clear aligners.
PAOO sets the stage for enhanced orthodontic movement by initiating selective alveolar decortications. This surgical step relies heavily on advanced piezoelectric devices and bone grafting materials to foster a conducive environment for rapid tooth adjustment. Once this strong foundation is established, Invisalign steps in to guide the teeth gently and effectively into their desired positions.
The integration begins with comprehensive assessments using CBCT scans, ensuring precise surgical intervention and tailored aligner fit. Following the PAOO procedure, Invisalign aligners are introduced typically within the two-week "golden window" where the Regional Acceleratory Phenomenon (RAP) is most active.5 This synergy captures RAP's peak period, enhancing the efficacy of the treatment.
Patients undergoing this combined treatment often express their satisfaction not just with the speed of results, but also with the comfort and aesthetics provided by Invisalign aligners. Since Invisalign trays are clear and removable, they maintain the patient's confidence and lifestyle with minimal disruptions. This approach appeals immensely to adults who desire discretion in their orthodontic journey.
One notable patient experience involves a 34-year-old woman presenting with a severe crossbite and Class III malocclusion. With PAOO and Invisalign, she achieved significant corrections in just 12 months. This case exemplifies how the synergy of these technologies shortens treatment durations while optimizing outcomes.
Functionally, Invisalign aligns with PAOO's accelerated movement capabilities, ensuring that teeth move confidently toward their target positions without compromising gum and periodontal health. The clear aligners provide a structured, controlled force that takes full advantage of PAOO's initial expedited movement.
Aesthetic benefits are equally noteworthy. Patients appreciate the virtually invisible nature of Invisalign. This appeals significantly to adults and teenagers who might otherwise feel self-conscious about metal braces. The combination expedites the journey to a healthier smile and maintains the patient's self-esteem and social comfort throughout the process.
Optimizing patient experiences extends beyond the initial treatment phase. Follow-up care ensures that the results achieved are maintained. Patients are educated on the importance of adhering strictly to their Invisalign regimen, regular oral hygiene practices, and scheduled dental check-ups. This holistic approach fortifies the stability of the corrections achieved through the PAOO and Invisalign combination.
The fusion of PAOO and Invisalign exemplifies how interdisciplinary advances in dental technology can offer superior, rapid, and comfortable treatment solutions. This integrated approach promises accelerated treatment times and a seamless, aesthetically pleasing experience that meets modern patients' demands for discretion and efficiency.
Potential Complications and Management
While periodontally accelerated osteogenic orthodontics (PAOO) offers significant benefits, it's crucial to manage potential complications effectively. The main concerns include:
- Root resorption
- Gingival recession
- Infection
Thorough preoperative assessments using diagnostic imaging like CBCT scans help identify pre-existing vulnerabilities and guide treatment planning. Balancing the force applied during tooth movement is essential to avoid excessive stress on the roots. Regular check-ups after the PAOO procedure enable early detection and intervention for root resorption.
Evaluating periodontal health before PAOO is vital to mitigate the risk of gingival recession. Soft tissue grafting can be integrated with PAOO if significant recession is observed. Postoperative care, including protective barriers and proper oral hygiene, further minimizes this risk. Educating patients about gentle brushing techniques and maintaining periodontal health is key.
Infection risks are inherent in surgical procedures. Strict sterilization protocols and prophylactic antibiotics reduce these risks. Postoperative monitoring for signs of infection and prompt intervention with appropriate antibiotics are crucial. Encouraging optimal oral hygiene and adherence to postoperative instructions prevents infections.
Patient education is pivotal in managing complications. Transparency about the procedure, benefits, and risks sets realistic expectations and fosters cooperation. Comprehensive preoperative and postoperative guidelines empower patients to take an active role in their care.
Scheduled postoperative visits allow for monitoring healing, assessing treatment effectiveness, and identifying emerging issues early. These visits reinforce patient education, ensure compliance, and enable necessary adjustments to the treatment plan.
Modern advancements and precise clinical practices significantly mitigate the risks associated with PAOO. Detailed preoperative assessments, strategic surgical techniques, and thorough postoperative care enhance the procedure's safety and success. Ongoing patient education and regular follow-ups ensure swift management of any complications, maintaining the patient's health and satisfaction throughout their orthodontic journey.
Future Directions and Research
The field of PAOO is brimming with promise as researchers and clinicians explore new avenues to refine and enhance this technique. Innovative materials, such as bioactive glass and nanomaterials, are being investigated for their potential to accelerate bone regeneration and enhance graft stability1.
Laser technology is another exciting development, offering more precise and less invasive corticotomy incisions compared to traditional surgical methods. Laser-assisted corticotomy may decrease patient discomfort and expedite healing, making PAOO even more patient-friendly2.
Electrostimulation, which uses low-level electrical currents to promote bone healing and regeneration, is being studied as a potential complement to PAOO. Preliminary research suggests that it could enhance the regional acceleratory phenomenon (RAP), resulting in quicker orthodontic adjustments3.
Advancements in imaging and simulation technologies, such as enhanced 3D imaging and AI-driven predictive modeling, enable more precise assessments and personalized treatment plans. Augmented reality (AR) could help orthodontists better visualize surgical plans and anticipated outcomes, ensuring heightened precision during procedures.
The application of growth factors and biomolecules, like bone morphogenetic proteins (BMPs) or platelet-derived growth factor (PDGF), to PAOO procedures is another promising area of research. By integrating these substances into graft materials, clinicians may expedite healing and enhance the quality of regenerated bone4.
Minimally invasive surgical techniques, such as piezocision or piezopuncture, offer less invasive alternatives to traditional corticotomy while still activating the RAP. These methods could expand PAOO accessibility to a broader patient demographic.
Researchers are also exploring the role of genetics and personalized medicine in PAOO outcomes. Understanding individual genetic predispositions could help customize the PAOO process more effectively to each patient's unique biology, potentially reducing variability in treatment outcomes and complication risks.
The convergence of PAOO with other orthodontic advancements, like self-ligating brackets or customized digital aligners, promises comprehensive treatment solutions that synergize multiple cutting-edge methodologies for quicker and more efficient results.
Continuous monitoring advancements, including smart wearables or intraoral sensors, could provide real-time data on tooth movement, bone density changes, and patient compliance, enabling more responsive and adaptive treatment adjustments.
Educational initiatives and interdisciplinary collaborations between periodontists, orthodontists, bioengineers, and materials scientists are vital for translating innovations in materials and techniques into clinical practice.
As PAOO advances, ongoing research and clinical trials are essential to validate new approaches and ensure their safety and effectiveness. The future of PAOO shines bright with the potential for even more rapid, efficient, and patient-centered orthodontic solutions that prioritize both health and satisfaction.
The advancements in PAOO demonstrate a commitment to improving patient outcomes through innovative techniques and materials. By accelerating treatment times and enhancing bone quality, PAOO represents a significant leap forward in orthodontic care. As research continues to evolve, the future of PAOO holds great promise for delivering efficient, patient-centered solutions that prioritize both health and satisfaction.